BLOG
Humeral Interlocking Nail Tips for Effective Fracture Healing?
The Humeral Interlocking Nail has gained attention in orthopedic surgery for treating humeral fractures. This implant effectively stabilizes the bone, facilitating fracture healing. By using interlocking screws, it provides enhanced locking capabilities, which improves stability during the healing process.
Despite its advantages, challenges remain. The ideal surgical technique is still debated among surgeons. Some report complications like infection or nonunion. Understanding the reasons behind these issues is crucial for improving outcomes. Further studies could illuminate best practices for using the Humeral Interlocking Nail effectively and safely.
Patient factors must also be considered. Bone quality, age, and activity level greatly influence healing. Customizing each approach can lead to better results. Reflecting on these variables is essential for optimizing fracture management with the Humeral Interlocking Nail.
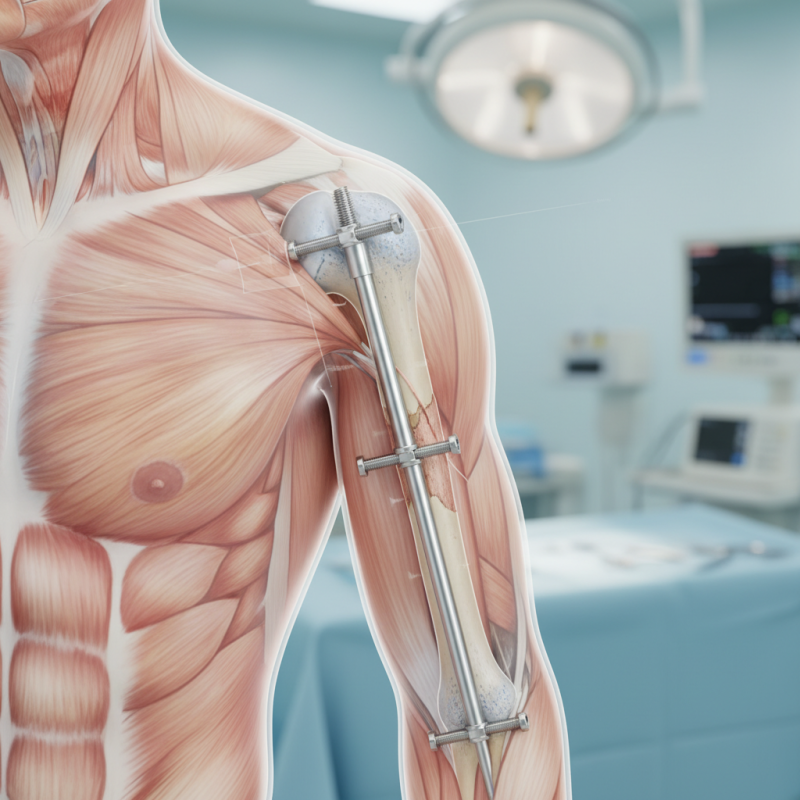
Understanding Humeral Fractures and Their Implications
Humeral fractures are common injuries, often resulting from falls or accidents. These fractures affect the upper arm and can impact daily activities. Understanding the nature of these fractures is crucial for effective treatment and rehabilitation.
Effective healing requires proper alignment of the fractured bone. Surgeons often use interlocking nails to stabilize the humerus. This technique enhances healing by providing support. However, it is essential to assess each case individually. Not all fractures are the same. Some may heal well without surgical intervention, while others require more aggressive treatment.
Rehabilitation plays a key role. Patients need to work on mobility and strength after the initial healing phase. Many face difficulties during recovery. Pain, stiffness, and frustration are common obstacles. Setting realistic goals is important. Progress may be slow, but consistent effort leads to improvement. Reflecting on one’s journey can offer insights into the healing process. Understanding humeral fractures promotes better outcomes and recovery experiences.
Overview of Interlocking Nail Technology in Orthopedic Surgery
Interlocking nail technology has transformed orthopedic surgery, specifically in treating humeral fractures. These nails provide stability, allowing for better alignment during the healing process. Surgeons can use them to facilitate quicker recovery times. However, issues such as infection risk and nail migration can still arise, indicating the technology is not flawless.
When applying interlocking nails, proper technique is critical. A well-prepared surgical field minimizes the risk of contamination. Ensuring the correct nail length and diameter is crucial for optimal results. It’s essential for orthopedic surgeons to address these concerns and refine their techniques. Research and training improve outcomes but may not eliminate all complications.
Incorporating patient education can also enhance recovery. Informing patients about their roles in post-surgical care helps reduce anxiety. Encouraging adherence to rehabilitation routines boosts healing. Surgeons must remain vigilant and adapt their methods as new challenges emerge in the evolving landscape of orthopedic surgery.
Techniques for Effective Humeral Interlocking Nail Placement
Humeral interlocking nails are critical for effective fracture management. Getting the placement right is crucial. Studies show that nearly 30% of patients experience some form of complication post-surgery. Precision can reduce these rates substantially. Effective techniques involve proper alignment and careful insertion. Surgeons must pay attention to the angling of the nail. Inaccurate placement can lead to nonunion or malunion.
Proper radiographic assessment is vital before the procedure. This step helps in visualizing the anatomy. The use of fluoroscopic guidance during insertion improves accuracy. According to recent data, fluoroscopy can enhance the overall success rate by 15%. Still, not all surgeons utilize this method. Some opt for manual alignment, which can lead to variability in outcomes.
Surgeons often face challenges with the soft tissue envelope around the humerus. An inadequate understanding of this area might cause complications. Limited exposure can hinder effective nail placement. Some techniques focus on minimizing soft tissue trauma, which is essential for recovery. There's a need to reflect on techniques adopted in various settings to improve outcomes continually.
Humeral Interlocking Nail Tips for Effective Fracture Healing
| Technique | Advantages | Considerations | Outcome |
|---|---|---|---|
| Closed Reduction | Minimally invasive, Lower infection risk | Requires good alignment | High fracture union rate |
| Open Reduction Internal Fixation (ORIF) | Direct access to fracture site, Precise fixation | Higher infection risk, Longer recovery | Effective for complex fractures |
| Intramedullary Nailing | Stable fixation, Allows early mobilization | Requires careful placement | Good functional outcomes |
| External Fixation | Minimally invasive, Can stabilize complex fractures | Risk of pin site infection, Aesthetic issues | Effective for temporary stabilization |
| Screws and Plates | Robust fixation, Versatile applications | Requires extensive soft tissue dissection | Excellent long-term outcomes |
Benefits of Humeral Interlocking Nails in Fracture Healing
Humeral interlocking nails have become a popular choice for aiding fracture healing. These innovative devices provide stability and support during recovery. When properly placed, they reduce the risk of malunion. This leads to more successful healing outcomes. Patients often experience faster recovery times, less pain, and greater mobility.
Here are some tips for considering humeral interlocking nails: Ensure you discuss potential complications with your doctor. Not all patients heal at the same rate. Some may face challenges, such as infections or stiffness. Clarity about your situation is crucial. Follow-up appointments are essential to monitor healing progress closely.
Another aspect to consider is rehabilitation. Physical therapy plays a significant role in recovery. It helps to regain strength and mobility. Remember, patience is key. Fracture healing is a process that requires time and dedication. If you push too hard, you might face setbacks that prolong recovery. Listening to your body is vital during this time.
Potential Complications and Challenges in Humeral Nail Surgery
Humeral nail surgery is frequently chosen for treating humeral fractures. However, several potential complications arise during this procedure. Infection rates range from 6% to 16%. These infections can lead to extended healing times and increased patient discomfort.
Another notable challenge is the risk of nonunion. Studies show nonunion occurs in approximately 10% of cases. Factors contributing to this issue include poor bone quality and inadequate stabilization. Surgeons must assess each patient's situation carefully. Pre-existing conditions can complicate healing further.
Hardware complications also pose significant risks. The failure rate for humeral nails can reach 20% in some studies. This often results in the need for additional surgeries. Patients may face long recovery periods, raising concerns about the overall effectiveness of the procedure. Reflecting on these challenges can enhance surgical practices and improve outcomes for future patients.

